This post is excerpted from my new book: Confronting the Cancer Care Plight: Using First Principles to Navigate Your Cancer Journey. Visit: myxcancer.com
Using the logic of life models, we replace aging cells with cancer cells
to construct a mathematical model. The total number of cancer cells is described by the following mathematical model:
when the total number of cancer cells reaches a certain proportion (i.e., the proportion of cancer cells to the total number of cells in the body), the patient will die. The goal of our cancer treatment is to clear cancer cells more effectively, preventing their total number from reaching the lethal proportion[1].
A treatment method without side effects might follow the pattern described below. When a cancer therapy can directly eliminate some cancer cells without any side effects, the patient will live longer after this treatment. The extension of life is directly proportional to the percentage of cancer cells removed. Although this therapy has no side effects, meaning it does not weaken the immune system's ability to fight cancer, it also does not enhance it. After a short-term decrease in the total number of cancer cells, their count will eventually begin to increase again, following the previous pattern.
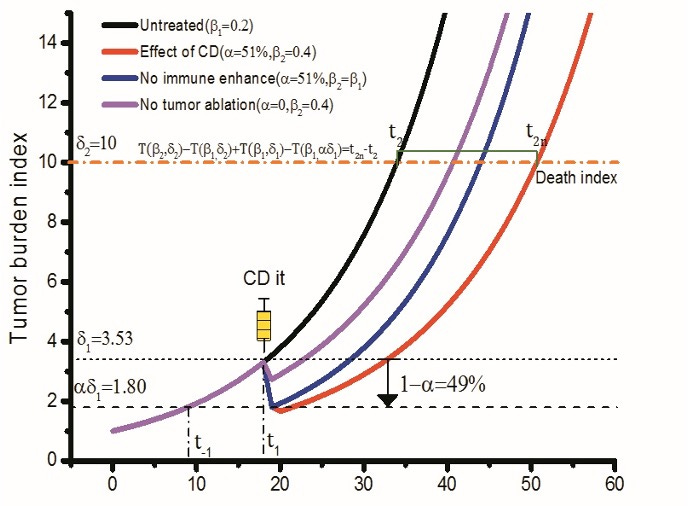
The diagram below models the treatment of cancer using a therapy known as CD cancer treatment. In this model, time is measured in days for mice and months for humans. A CD therapy is administered when the tumor reaches a specific size, with a set point for when it becomes lethal. This treatment directly reduces the tumor size and enhances immune function. As a result, the tumor is reduced to 51% of its original size, effectively shifting the progression of the tumor earlier by several periods, which delays the advancement of the disease.
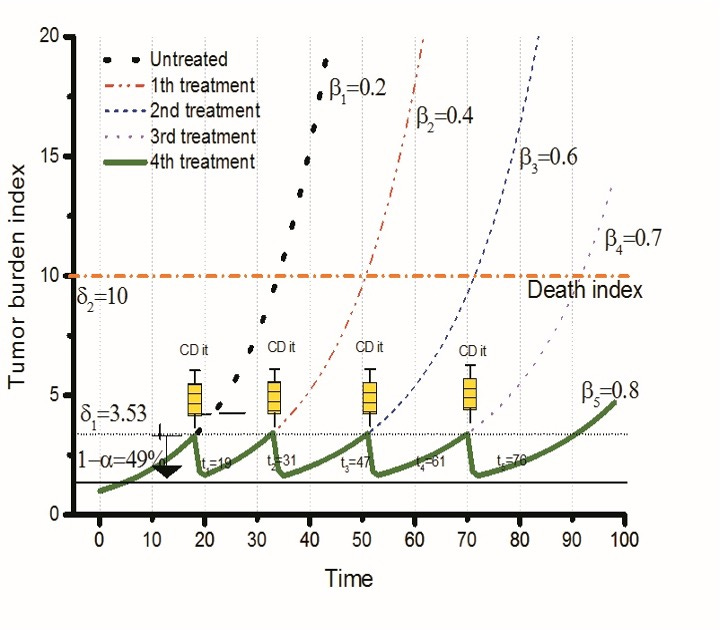
If a cancer treatment method can be used continuously and reapplied before the total number of cancer cells crosses the mortality threshold, ideally each treatment would also enhance the immune system's ability to eliminate cancer cells. Theoretically, this approach could extend a patient's life indefinitely, as illustrated in the figure below.
For a treatment to be sustainable, it must not lead to drug resistance. In the Further Reading section, we have refined our model to include variables for drug resistance. When a therapy develops resistance, the cancer treatment model undergoes significant changes. Simply eliminating cancer cells is not the best strategy; it is more effective to maintain sensitive cancer cells within a controlled range rather than completely killing them off. This is because cancer cells compete with each other, and eliminating all sensitive cells provides space and nutrients that accelerate the growth of resistant cells. This concept can be explained by the ecological dynamics in Siberia, where deer, wolves, and tigers coexist. Initially, hunting tigers to increase deer populations led to an increase in wolves and a decrease in deer. Later, banning tiger hunting allowed tiger populations to recover, which in turn decreased wolves and increased deer. When multiple competitors exist, eliminating one can inadvertently increase the others.
Even without mathematical models, we can deduce that resistance is a serious problem in cancer treatment, leading to unsustainable therapies and leaving patients in advanced stages without viable treatment options. Most current cancer therapies face some level of resistance. Research indicates that even physical methods like radiation therapy develop resistance. Targeted drugs are inherently resistant, as they are designed to attack cancer cells with specific mutations. Due to the heterogeneity of cancer, mutations are numerous, and targeted drugs can only kill a subset of sensitive cells, not the resistant ones. Even immunotherapies, such as PD-1 inhibitors, exhibit some resistance. Any therapy that selectively kills certain types of cancer cells is inherently prone to resistance and often cannot be used continuously.
While drug resistance is a major factor in the sustainability of cancer treatment, other factors also play a significant role. For example, surgery poses similar challenges to sustainability. It's clear that cancer surgeries, especially radical surgeries that remove entire organs, are difficult to repeat. Not only do these surgeries aim to remove all cancerous tissues, they often also remove some healthy tissue, making repeated surgeries less feasible.
Using cancer models, we can identify five key factors that are crucial for achieving the ultimate goals of cancer treatment. These factors are: efficacy(or inhibition rate), safety, resistance, sustainability, and convenience. Each of these plays a critical role in determining whether cancer treatment can be successful in the long term.
6.1 Efficacy (or Inhibition Rate)
Efficacy refers to the rate at which cancer cells are eliminated; a high efficacy indicates that the cancer treatment is highly effective at killing cancer cells. In cancer treatment, efficacy is the simplest and most common measure, and it is often the primary goal of almost all cancer therapies. Many new treatments even set efficacy as their sole target. A clinical trial can prove a treatment or new drug effective by achieving just one clinical endpoint, and efficacy is the easiest effect to observe in the short term. However, once a treatment or drug is approved, other critical variables like safety might be overlooked.
While a higher efficacy is always desirable, it should not be pursued at the expense of other attributes. Efficacy is crucial, but it is not everything.
In our life model, we discuss two pathways to clear senescent cells: one is direct elimination through specific therapies, and the other enhances the immune system's capability to naturally engage in the clearance process. Similarly, in our cancer model, there are two pathways to eliminate cancer cells: direct removal and activating the immune system to enhance its ability to clear cancer cells.
For cancer patients choosing a treatment plan, it's essential to consider the efficacy of the recommended therapies or drugs, which could stem from direct clearance, reliance on the immune system, or a combination of both. A treatment that offers both direct clearance capabilities and the ability to activate the immune system for a systemic elimination of cancer cells should be preferred. For example, surgical tumor removal typically only directly clears cancer cells and rarely boosts immune function. In contrast, many interventional ablation procedures not only directly ablate cancer cells but also release tumor antigens that enhance the immune system's anticancer capabilities. Given similar conditions, cancer patients should prefer interventional ablation procedures.
6.2 Safety
Safety in cancer treatment, particularly regarding the side effects of therapies, is crucial. While the threshold for tolerating side effects in developing cancer therapies is high, this does not imply that safety concerns can be overlooked. For cancer patients, side effects that are not life-threatening may seem minor compared to the prospect of death. However, since most cancer drugs fundamentally act as poisons due to their toxic properties, doctors often view side effects as an unavoidable consequence.
In many cases, cancer patients might overlook the side effects of their treatments. However, they may later discover side effects that severely impact their quality of life. For example, 80% of patients who undergo hysterectomy develop neurogenic bladder, a form of urinary incontinence, which in severe cases can lead to hydronephrosis and kidney failure. Annually, about 2.5 million hysterectomies are performed in China and approximately 400,000 in the United States. Most of these patients experience urinary system issues because radical surgeries aimed at removing all cancerous tissues can easily damage internal nerves.
Furthermore, nearly 100% of patients undergoing chemotherapy experience various side effects, with 80% suffering from severe anemia. The side effects of cancer treatment seem to be the cost of high efficacy, but it is crucial to recognize that most of these side effects damage the immune system, reducing or eliminating the body's natural anticancer immune capabilities, thus increasing the likelihood of cancer recurrence. Clearly, these side effects are not worth the trade-off, as the true goal for patients is not short-term cancer suppression, but a longer, healthier life. Sacrificing long-term benefits for short-term high efficacy by damaging the immune system is not justified.
The human immune system plays a continuous role in fighting cancer, even when cancer is present. The immune system is a natural anticancer tool, and if future treatments damage this system, the patient's future becomes bleaker, with short-term cancer suppression potentially shortening rather than extending life.
When choosing therapies for cancer patients, while it might be impossible to find treatments or drugs without any side effects, those with fewer side effects and higher safety should be prioritized. For instance, the side effects of chemotherapy drugs largely stem from their systemic application, spreading toxic substances throughout the body. I am aware of a private hospital in China, named after its founder Bofa Hospital, which has adopted a new method of drug delivery by injecting chemotherapy drugs directly into the tumor. This approach significantly reduces side effects while maintaining the desired inhibitory effects of chemotherapy, potentially offering higher efficacy than traditional methods.
6.3 Drug Resistance
While drug resistance differs from safety concerns, the outcomes can be similar. In the pursuit of high short-term suppression rates, clinical trials often limit their focus to a subset of patients with high mutations in specific targets, which almost invariably leads to drug resistance. We've discussed how overly complex technological solutions can lead to more problems before fully understanding the relationship between genetic mutations and cellular changes. Short-term fixes targeting genetic mutations can lead to more complex long-term issues. In applying first principles to complex problems, it's crucial to avoid falling into the trap of reductionism, which involves breaking down problems to an excessively detailed level. Since there's still much uncertainty below the cellular level, it's sufficient to break down the basic components of cancer treatment to the cellular level.
The medical research community often prides itself on using complex technologies, which inevitably lead to complex issues such as drug resistance. Unfortunately, cancer patients and doctors, who are guided by established guidelines, are often powerless to change this trend. However, as patients, we can choose treatments with lower or no resistance from the options provided by doctors.
The fundamental cause of drug resistance is that treatments or drugs selectively kill only those cancer cells sensitive to them. Once there are no sensitive cells left in the cancer tissue, the treatment or drug can no longer suppress the malignant proliferation of the cancer. Although cancer cells share certain characteristics, each cancer tissue is heterogeneous, characterized by hundreds of mutations. Targeting drugs that focus on a single mutation can only kill a subset of cancer cells. However, drugs like Gleevec have shown much better results for certain blood cancers with a singular mutation profile. Since its release in 2001, Gleevec has shown an effectiveness rate of over 94% in treating chronic myeloid leukemia, with 76% of patients returning to normal levels and ratios of various blood cells.
However, such cancers are not common, and most cancers, particularly solid tumors, are characterized by their heterogeneity and resistance to targeted drugs. While it might seem feasible to gradually develop targeted drugs for various mutations, it's not that simple. In our cancer models, we see that once a targeted drug develops resistance, it no longer suppresses resistant cancer cells. Instead, by eliminating competitive cancer cells, it allows resistant cells to proliferate more rapidly. Essentially, while the drug might reduce the size of the tumor in the short term, it actually shortens the patient's life. [2]
Similar to how some side effects merely reduce the quality of life while others can hasten death, drug resistance can paradoxically shorten life if targeted drugs effectively reduce tumor size in the short term but ultimately fail to extend the patient's life. This contradicts the ultimate goal of cancer treatment. Without applying first principles, such outcomes might become the norm, as both patients and doctors favor using complex, newly developed targeted and immunotherapeutic drugs.
By applying first principles, we would be particularly cautious in using drugs developed through complex molecular biology technologies. We should focus on the cellular level to use these drugs wisely and minimize their resistance, perhaps by maintaining a controlled number of sensitive cancer cells rather than eliminating them all, which can also suppress the proliferation of resistant cells. Additionally, we should reevaluate our models of cancer progression to consider both suppression rates and resistance, balancing short-term effects with long-term benefits and choosing treatments with a lower incidence of resistance.
6.4 Sustainability
Safety and drug resistance are major factors contributing to the unsustainability of cancer treatments. If the side effects of a cancer treatment are severe enough, they may prematurely end a patient's life; similarly, using the latest drug-resistant treatment methods might also shorten a patient's lifespan. Once a patient has passed away or is near death, not only is the treatment they were using no longer viable, but they are also unable to choose other cancer treatment options. Thus, we define the sustainability of cancer treatment as the ability to continue using a treatment method that consistently kills cancer cells, keeps the cancer burden below a lethal threshold, and extends the patient’s life. Clearly, the sustainability of cancer treatment is a crucial component of cancer treatment goals and is indispensable.
Safety and drug resistance directly impact the sustainability of cancer treatments, which is easy to understand. However, there are also sustainable factors that are neither related to safety nor resistance but still affect the sustainability of cancer treatments. For example, surgical removal of cancer, which has almost no sustainability. If cancer is detected early and the lesion is relatively small, doctors generally recommend surgical removal. In the real medical environment, doctors tend to remove a larger portion of normal tissue to ensure that the cancer is completely excised. Surgical procedures are unlikely to stimulate the immune system to engage in anti-cancer activities, and without an enhanced immune system, the likelihood of cancer recurrence is high, regardless of whether there are residual cancer cells. Facing recurrent cancer, it is almost impossible for patients to undergo the same surgical removal again.
In cancer models, early detection and treatment indeed can increase patient survival, but this is under the assumption that there are no side effects or resistance. It is generally believed that small cancer surgeries effectively remove cancerous tissues without side effects or resistance. Therefore, guidelines advocating for early detection and treatment are based on the suitability of surgical removal for early-detected cancers. However, even if the sustainability of surgery is low, early detection and treatment do not necessarily benefit patients in the long term, and the extended survival period from early detection and treatment may not be as beneficial as other cancer treatments that are not based on early detection.
Understanding this perspective, let's consider a scenario: if a cancer patient misses the opportunity for early detection and surgical treatment, and the cancer is discovered too late for surgery, the patient can still choose other treatments similar to surgery, such as local tumor ablation. Local tumor ablation can not only kill the entire cancerous tissue like surgery but also has a proven benefit of stimulating the immune system's systemic anti-tumor capabilities.
When choosing a cancer treatment, patients must give considerable importance to the future sustainability of cancer treatments. In approved cancer treatments or when choosing better options from the NCCN guidelines, patients can still select sustainable cancer treatments based on our cancer model's systemic thinking (i.e., first principles).
6.5 Convenience
In the healthcare system, while convenience may not be as critical as other factors, it significantly influences patients' choices. Patients are likely to opt for more convenient treatments if other conditions are similar. Generally, convenience implies cost-effectiveness and sustainability. Once cancer patients enter a hospital, it must be acknowledged that most hospitals are motivated to recommend the latest and most expensive cancer treatments, often overlooking convenience in their decision-making. Even under guidelines that promote early detection and treatment, patients are typically advised to undergo complex surgeries rather than more convenient minimally invasive ablations. This is because a hospital may not be proficient in all cancer treatments and tends to adopt the latest and most complex technologies. Additionally, convenience is often associated with lower cost and perceived lower quality. For instance, In China, the cost of a cancer surgery is around $10,000, whereas the same tumor treated with radiofrequency ablation costs about $5,000. Local ablation procedures have fewer side effects and better immune activation compared to surgical excisions. Despite this, the number of patients choosing surgery significantly exceeds those opting for radiofrequency ablation.
Of course, the issue of convenience is less critical than other factors, and as technology advances, many cutting-edge techniques are making cancer treatments more convenient. For example, advancements in modern imaging equipment like CT, ultrasound, and MRI have simplified previously complex cancer treatments. Moreover, choosing convenient treatments does not necessarily mean sacrificing other metrics. While most oral medications are less effective than intravenous drugs, technological advancements have enabled highly effective treatments that offer convenience comparable to, or even better than, traditional methods. For instance, traditional radiotherapy has evolved into more effective proton or heavy ion therapy, and treatments that involve directly inserting radioactive materials into tumors are more convenient and as safe as proton therapy.
In summary, while convenience might limit some effective cancer treatments, the essence of first principles is to simplify complex problems. When applying first principles, convenience should not be considered in isolation but integrated with other metrics to make informed decisions about cancer treatment options. Particularly, decisions based solely on convenience are likely not optimal as its correlation with other important factors might be weak.
[1] For readers with a mathematical background, you can explore the Further Reading section of this book, which contains the full content of the mathematical model of cancer.
[2] The mathematical model shown in the figure below can be found in the Further Reading section. In this model, the initial tumor burden index (V0) is set at 3.3 at the start of cancer treatment. When treatment begins with a drug that causes resistance, a higher dosage results in more significant tumor reduction but a shorter extension of the patient's expected survival time. Conversely, reducing the drug dosage to a level that only maintains the non-proliferation of sensitive cancer cells without shrinking them results in a longer expected survival time. This model applies to a scenario where the proportion of drug-sensitive cancer cells is low, with (s = 0.5).



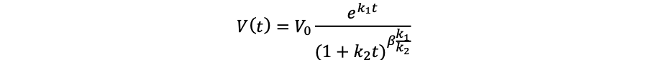

Very good 👍👍